There’s no doubt that as a doula, your clients and others in your community look to you for information surrounding pregnancy, birth and the transition into parenthood.
Common Pelvic Floor and Core Issues
As a pelvic health physiotherapist with a focus on prenatal and postpartum care, I hear daily from expecting and new moms – ‘why did no one tell me?’ – referring to the MANY common pelvic floor and core issues that can occur.
- 1 in 4 women will experience urinary incontinence (1)
- 50% of women will experience a degree of pelvic organ prolapse in their life (2)
- 62% of women experience dyspareunia (pain with intercourse/penetration) during the first three months postpartum (3)
Instead, women tend to hear from family, friends and even medical providers that leaking urine/stool/gas, pelvic pain, back pain, pubic bone pain are all a normal part of pregnancy and that surgery is the only answer. No person deserves to live with these symptoms. Pregnancy and birth are not an excuse to put up with them!
Here are 7 pelvic health tips to help empower you and prepare clients for the best possible
outcomes during pregnancy, birth and beyond!
1: Get familiar with the pelvic floor and core
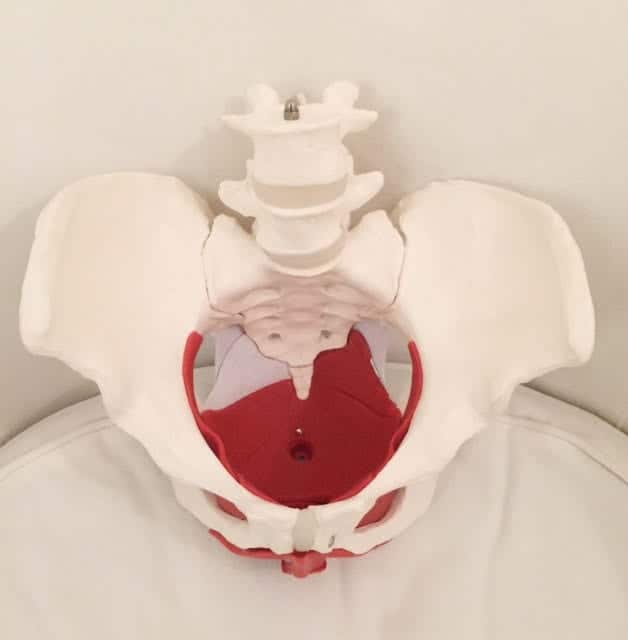
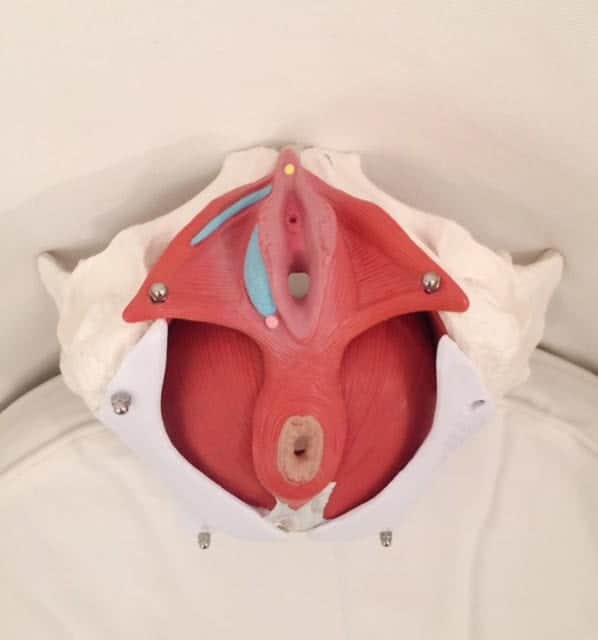
Start with an explanation of where our pelvic floor muscles are (yes, many people have no idea because this area of the body is often considered inappropriate to talk about… let’s change this!). The pelvic floor muscles attach from your pubic bone to tail bone (front to back) and sitz bones (side to side). They have many jobs including supporting your bladder/uterus/rectum (and your baby when pregnant), supporting your low back/pelvis/tailbone, have a sexual role, are a part of our breathing system and close the openings where urine and stool/gas come out to prevent us from leaking.
Our inner core is like a canister; the diaphragm (deep breathing muscle) on top, transversus abdominis (corset type muscle) wraps around the center, the pelvic floor is the bottom and then multifidus muscles that attach along our spine.
It’s important to know that the pelvic floor doesn’t work in isolation which is why those good ole kegels aren’t always the answer. If you were to pick up a bag of groceries – it’s not just one muscle doing all of the work, so if we want to stop leaking urine, why should it just be one muscle’s job?
Check out this video to find out more about how your core and pelvic floor work and tips your clients can start doing today!
2: Kegels aren’t always the answer
Often when anything is mentioned about what to do with the pelvic floor – it’s ‘go do kegels’ BUT did you know many women aren’t finding the right muscles and sometimes these muscles are actually tense and need to be released instead of strengthened?
Seeing a pelvic health physiotherapist during pregnancy can help you learn how to increase strength or release tension in your pelvic floor/core and prepare your body for birth and postpartum recovery.
Whether you’re three months, three years or thirty years postpartum, it’s never too late to see a pelvic health physiotherapist to resolve pelvic health symptoms.
For a more effective way to engage your inner core canister – check out these two techniques (piston breath /core breath) which don’t just isolate your pelvic floor like a kegel.
Research shows that pelvic floor muscle training should be the first recommended type of treatment for women with urinary incontinence. Pelvic health physiotherapists are qualified to carry out internal assessment and treatment of the pelvic floor which has been shown to be 80% effective at improving and curing urinary incontinence (4).
For clients who can’t see a pelvic health physiotherapist, here are some helpful prenatal and postpartum online resources:
Julie Wiebe – The pelvic floor piston: foundation for fitness
3: Use the breath to relax the pelvic floor during labour.
Specifically for birth, I teach my clients to release tension in their pelvic floor using the Flower Bloom Breath. This is a breath that as their birth doula – you can teach them during pregnancy and remind them throughout labour.
I can’t tell you how many of the postpartum moms I see say this breath was a huge part of what got them through each surge/contraction as well as the second stage of labour.
4: Encourage perineal massage to decrease risk of trauma to the pelvic floor and prepare mentally for birth
Some prenatal education classes teach about perineal massage while others don’t mention the pelvic floor at all. Now you can empower your clients with up-to-date information of why perineal massage may be helpful and two helpful perineal massage techniques.
Perineal massage may be most effective for first time mom’s to help decrease risk of perineal trauma (tearing or episiotomy) (5) but many new and experienced mom’s find it helps them also mentally prepare for birth.
I recommend clients start around 35 weeks into pregnancy. It can be challenging to reach their perineum area so if they have a partner, it can be helpful to have them do the massage while your client focuses on using the flower bloom breath (from Tip 3). Have your client check with their care provider to be sure perineal massage is appropriate for them.
5: Combine spontaneous pushing with a sidelying birth position to decrease risk of tearing.
When looking at the effects on the pelvic floor, directed pushing can cause the mom to become physically exhausted sooner and may result in perineum tearing and a weaker pelvic floor postpartum, whereas spontaneous pushing can lessen the chance of trauma to the perineum and pelvic floor muscles (6).
When comparing lying on the back vs gravity neutral positions such as hands and knees or sidelying for pushing – the latter can help ease back pain and sidelying in particular is associated with lower risk of perineum tearing and can often be an option even with an epidural (6, 7, 8).
6: Use pelvic floor and core healing products to help with postpartum recovery
These postpartum healing products can help in your client’s recovery and boost their confidence going into birth:
1. – sitz bath
2. – sitz bath herbs
3. – perineal spray
4. – witch hazel for postpartum pads (or padsicles)
(To find out how to use these postpartum healing items – here’s a quick video)
Some women find using an abdominal wrap or having postpartum support shorts during the first eight weeks postpartum helpful to offer support while their inner core is healing (should feel like a gentle hug NOT a corset). It’s important to not just rely on the wrap/shorts for support but to begin some gentle inner core activations (see Tip 2) during their day to help restore their core from the inside out.
7: Promote pelvic floor and core healing early postpartum
Regardless of if your client had a vaginal or cesarean birth, the pelvic floor and core have gone through changes and need TLC before returning to high intense and high impact exercise.
During the first 6-8 weeks postpartum:
- Gradually increase walking, resting when possible
- Be mindful of rib over pelvis posture to help the core canister restore
- Add core breath/ piston breath (see Tip 2) and eventually progress to adding other exercises such as squats and lunges
- Have an assessment with a pelvic health physiotherapist to check how your core and pelvic floor is healing and to guide you back to your activity goals symptom free
Check out the online core exercise resources in Tip 2 that can be used postpartum.
Most women will have a six week follow up with their doctor/midwife where they get the ‘green light to exercise’ BUT their pelvic floor and core are rarely assessed internally and so they jump back into running, bootcamp and often ongoing pelvic floor symptoms continue or begin to happen.
Seeing a pelvic health physiotherapist at this time can positively impact your client’s pelvic floor and core healing and increase their self-confidence for returning to their goals.
Your clients are going to appreciate your recommendations when it comes to pelvic health which will empower them with knowledge that pelvic health issues don’t need to be their new normal.
Connecting with a pelvic health physiotherapist in your community can greatly benefit your clients. Having done specific birth doula training for physiotherapists, I discuss the option of having a doula with all of my prenatal clients and explain the beneficial evidence behind the amazing support you can offer.
Many expecting moms want to learn how to prepare for birth so I’ve put together my top 7 tips to help prepare for a positive, fear free birth in a free e-resource guide that you and your clients can access here. Of course one of my top tips is to have a doula – I can’t rave enough about having a maternal support practitioner!
Please share these resources with your clients and let’s work together to create more positive pregnancy, birth and postpartum experiences!
Anita Lambert, MSc (PT), BKin (Hon), PMA®-CPT
Anita Lambert is a Pelvic Health and Orthopaedic Physiotherapist with a focus on prenatal and postpartum. She graduated from McMaster University with an Honours Bachelor of Kinesiology and a Masters of Science in Physiotherapy. Anita is one of the select few physiotherapists in Canada to receive advanced training in labour support, which blends orthopaedic physiotherapy expertise with birth doula support.
Anita’s practice, Holistic Health Physiotherapy in Peterboroughn Ontario, is focused on guiding women to prevent and heal physical ailments that are common but shouldn’t be considered their ‘new normal’ during fertility, pregnancy or postpartum stages of life as well as help prepare for a positive birth experience.
www.holistichealthphysio.com
[email protected] FB: @HolisticHealthPhysio
IG: @HolisticHealthPhysio
TW: @Holistic_physio
References:
- (n.d). The Canadian Continence Foundation. Retrieved August 23, 2017, from http://www.canadiancontinence.ca
- Hagen S, Stark D. Conservative prevention and management of pelvic organ prolapse in women. Cochrane Database Syst Rev. 2006 Oct 18;(4):CD003882.
- Barrett G et al. Women’s sexual health after childbirth. BJOG 2000;107:186–95.
- Dumoulin C, Hay-Smith J et al. Pelvic floor muscle training versus no treatment, or inactive control treatments, for urinary incontinence in women: a short version Cochrane systematic review with meta-analysis. Neurourol Urodyn. 2015 Apr:34(4):300- 8.
- Beckmann MM, Stock OM. Antenatal perineal massage for reducing perineal trauma. Cochrane Database Syst Rev. 2013 Apr 30:(1):DOI: 10.1002/14651858.CD005123.pub3.
- DiFranco JT, et al. Care Practice #5: Spontaneous pushing in upright or gravity-neutral positions. J of Perinat Educ. 2007 Summer; 16(3):35-38.
- Shorten A et al. Birth position, accoucheur, and perineal outcomes: informing women about choices in vaginal birth. Birth. 2002; Mar:29(1):18-27.
- Soong B, Barnes M. Maternal position at midwife-attended birth and perineal trauma: is there an association? Birth. 2005; Sep:32(3):164-9.
You might also like:
Sorry, we couldn't find any posts. Please try a different search.

FREE ONLINE MINI-COURSE
BLISS IN BUSINESS RETREAT
Your future is created by what you do today — that's why we created a completely FREE mindset mini-course to help doulas and birth workers find bliss in their business!



Thank-you for all the info and easy accessibility to these resources. I can definitely see myself referencing this article in the future!